Ok, it has been a month and a half. We (Jody and I) have found the YANANOW site a very valuable resource. We think that a brief past history of my health is of import to this blog. We will compile this later on. However by way of introduction please find the following google doc links. Images and other links to be added.
A brief personal history is of importance to the prevention of Cancer. The medical industry focuses on the diction and cure of cancer as a profit center. OHSU takes a passing interest even in my past or current diet or activities. In other words, Cancer treatment is not from our point of view personal.
We (Jody and I) are rather disturbed about this. Interview - "The Secret History of the War on Cancer" gives a view of why prevention is of such importance. If you want to prevent the return of Cancer gets the audio-book. The scope of the book is incredible it's a long read. We suggest the audio-book. It is available for free through you local or not so local library.
Interview with the author - https://www.youtube.com/watch?v=uKsf6WtvxEE
Before the Cancer diagnosis, we listened to "the emperor of all maladies" audio-book. The history is as gruesome as it is interesting. Winner of the Pulitzer Prize, and now a documentary from Ken Burns on PBS, A must see if you have Cancer of any type.
http://www.pbs.org/show/story-cancer-emperor-all-maladies/
We feel it's important for people with Cancer to understand the history. We have found the current state of treatment of Cancer is only a little better now as in the past. The general prostate Cancer treatment is to kill it by cutting, sunburn, or cooking it.
The links to the medical documentation:
PSA History graph:
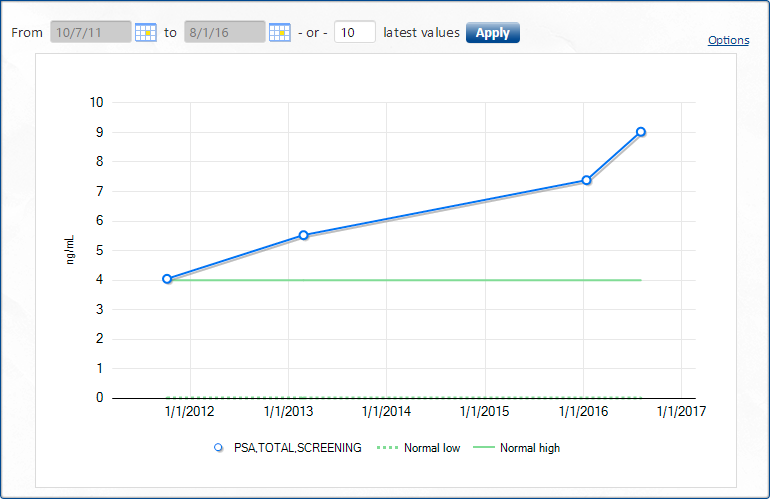
You can see the jump in the PSA. I was lucky to get an MRI done before a biopsy was done. The MRI-guided the biopsy. If I had not had the MRI images cancer would not have been found at all. See a description of biopsy below the MRI report.
The detail report from the Magnetic Resonance Imaging MRI with a rather large coil / antenna in my rectum. Using meditation I was able to not move a twitch resulting in very good images.
It is of great importance to learn how to read and understand this report. Below is a copy of my MRI. One of the things to important to notice is the Cancer is in only one location. It seems to start in my right nerve bundle and is moving out from that location. This means it most likely is caused by industrial exposure cadmium over 30 years ago.
A large tumor was found it turned out not to be Cancer. However I was lucky again if the tumor was not found the biopsy would not have been done. Wow...
- EXAM: MRI Prostate with and without intravenous contrast.
- HISTORY: Elevated PSA=9, evaluate for prostate cancer
- COMPARISON: None.
- TECHNIQUE: Endorectal multiparametric and multiplanar MRI of the prostate
- performed, including axial T1 images of the pelvis and high resolution axial
- T2, diffusion, and perfusion pre-and post dynamic intravenous gadolinium images
- of the prostate.
- FINDINGS:
- The prostate measures 5.7 CM transverse by 4.9 CM anteroposterior by 5.9 CM
- craniocaudal, giving a gland volume of 85 mL . No post-biopsy hemorrhage noted
- on T1 weighted images.
- A dominant tumor focus is identified in the right anterior central gland,
- measuring 1.4 CM transverse by 2 CM anteroposterior by 2.6 CM craniocaudal,
- giving a tumor volume of 3.8 mL . The tumor demonstrates:
- Low T2 signal: Yes, mildly heterogeneous.
- Restricted diffusion: Yes, mildly heterogenous hypointense signal .
- Early enhancement: Yes.
- Delayed washout: No.
- Overall Pi-RADS classification:
- 4, based on the T2 and ADC heterogeneity.
- With respect to tumor stage:
- Likelihood of right-sided extracapsular extension: Absent (0-20%).
- Likelihood of left-sided extracapsular extension: Absent (0-20%).
- Likelihood of right-sided seminal vesicle invasion: Absent (0-20%).
- Likelihood of left-sided seminal vesicle invasion: Absent (0-20%).
- A peripheral left central gland focus at the base of the prostate with
- heterogenous diffusion restriction and washout is encapsulated and compatible
- with a BPH nodule. Urinary bladder trabeculations are noted secondary to
- chronic bladder obstruction. No lymphadenopathy, suspicious bone lesions, or
- other abnormality identified.
- IMPRESSION:
- 1. Dominant right paramedian anterior central gland PI-RADS 4 focus, suspicious
- for malignancy. This is amenable to direct of fusion guided biopsy.
- 2. Moderate prostatomegaly, with changes of benign prostatic hyperplasia.
- Recent literature on likelihood of prostate cancer by scenario:
- Repeat biopsy positive in 5 of 112 patients (4.5%) with negative MRI and prior
- negative TRUS biopsy (J Urol 2014; 192: 60-66).
- Repeat biopsy positive in 47 of 58 patients (81.0%) with positive MRI and prior
- negative TRUS biopsy (J Urol 2014; 192: 60-66).
- Biopsy positive in 33 of 151 (21.8%) low risk biopsy naive patients (PSA < 10
- and negative digital rectal exam) with negative MRI (J Urol 2013; 190: 502-8).
- Biopsy positive in 23 of 43 (53.4%) high risk biopsy naive patients (PSA > 10
- or positive digital rectal exam) with negative MRI (J Urol 2013; 190: 502-8).
- Biopsy positive in 53 of 94 (56.4%) low risk biopsy naive patients (PSA < 10
- and negative digital rectal exam) with positive MRI (J Urol 2013; 190: 502-8).
- Biopsy positive in 48 of 63 (76.1%) high risk biopsy naive patients (PSA > 10
- or positive digital rectal exam) with positive MRI (J Urol 2013; 190: 502-8).
Attending Radiologists: JOYCE MHLANGA, MBBCH
Author: APURVA BONDE, MD
I personally reviewed the images and, if necessary, edited the report. I agree with the report as now presented.
BIOPSY
An MRI should be a standard procedure done before a biopsy. I would have had the typical 12 core biopsy that leaves the lower section (hard to get at) unsampled. So I had a 19 core biopsy (7 more cores lower that a typical biopsy was taken) or cancer would not have been detected.
One of the things to important to notice in the biopsy below is the Cancer is in only one location. It seems to start in my right nerve bundle and is moving out from that location. This means it most likely is caused by industrial exposure cadmium over 30 years ago.
Summary:
1. Have an MRI before a biopsy ... force them to... it should be standard procedure.
2. The standard 12 core biopsy is missing early cancer. Have a 19 added lower than the standard procedure. This has really saved my life ... I am very lucky. Important contamination / small particles /toxins enter the pancreas by traveling down the nerve bundles.
3. Learn how to read your biopsy and keep track. We found doctors report that stated a 3-4 condition when the biopsy stated a 4-3. Its a big difference. We have had to correct doctors mistakes several times. You must take active care of your self.
Conclusion:
A strong immune system kills cancer. If the immune system is damage Cancer can exist. however Cancer can only grow if the testosterone promotes growth. It allows the cancer to grow blood vessels (this is called angiogensis). Turning off the blood vessel growth can be done by diet. Angiogenesis inhibitors / anti-angiogenesis food prohibit cancer from growing blood vessels. I have had for several years an anti-angiogenesis diet. Thus its a good bet the Cancer I have has evolved to promote its own growth in response to my diet. Citations / links for the above claims in next update.
Please excuse the long length of time before checking in. Right off, I want to say that Yananow was absolutely primary in my being able to make the right decision for me. The database comparison is brilliant and the reference material invaluable. The candid personal histories and sharing are so incredibly supportive … I can not thank you all enough.
Here is a summary of my results:
After lots of research, especially by my loving partner, we almost chose Calypso radiation therapy, until we were told it would be in conjunction with hormone replacement therapy. I did not want to go that route, because I have had some heart issues which I have stabilized through diet and exercise, and HRT seems risky for the heart from various research we read.
Consequently, I was fortunate to be the patient of Dr. James Porter at Swedish Urology in Seattle, WA, for the DaVinci robotic surgery to remove my prostate and hopefully the cancer. BTW, check out propublica.org. This site rates US surgeons and hospitals effectiveness on various procedures from public Medicare data, for example - return rate due to complications.
I had a PSA of 9 with a 4+3 prior to surgery. My prostate was 90 grams, the cancer was 3 grams. The cancer was in the lower right below the pelvic bone near the nerve bundles. The cancer was not near the margins of the prostate. Dr. Porter was able to spare my nerve bundles. The pathology report after surgery downgraded me to a 3+4. PSA levels are now undetectable.
The normal pattern and position of a 12 needle biopsy would not have found my cancer, because the cancer was located much lower. An additional 7 needles were added to the 12, and consequently cancer was detected.
7 additional needles were used, because an initial MRI had been taken and it showed a tumor in that area. However, the tumor was a benign fibroid tumor. I should add that an MRI prior to biopsy is not usual, but my wife and I were leaving the US indefinitely for our home in Chile in a few days. So, my doctor ordered an MRI before we cancelled our tickets.
So it was indeed a great deal of luck that my cancer was found.
As far as urinating goes: I have had control as soon as I removed the catheter. This I am told is unusual. I was surprised that I did not have more trouble. I wore light pads for 2 months anyway. There is a feeling of urgency, and there were two times in which I lost some control and dribbled a little.
As far as sexual climax goes, I have not tried any devices or drugs. I have had erections starting in the third week. With the prostate gone, there is no ejaculate. Oral stimulation to reach a climax works well. The first one was like an electrical shock and was painful. The second was better. A few months later, with a little creativity and flexibility, sex for both of us is very satisfying but a somewhat different experience. I am very fortunate to have a best friend and lover of 50 years.
As far as the recovery pain. The first three days were really bad. Dr. Porter said narcotics would slow the healing process, so I took Tylenol only to go to sleep for several hours, then wake up from pain. Next two hours walk around but not too much, sit down, eat just a little; easily digestible food is necessary. Empty the bag, wait for the pain meds to work, go to sleep. The fourth day, I was able to sleep a full 8 hours and have a normal day.
The first couple days, there was a great deal of reference pain in my shoulders from the CO2 gas used during the operation. This was a total surprise to me. The pain in my shoulders was very intense. I had not heard about the use of CO2 gas to inflate the body for laparoscopic surgery.
For me, there was no pain / burning from the catheter, though I have heard that is often the case.
Ok the big big surprise. It seems that the 90 gram prostate was perhaps causing problems with my intestinal process. I was leaking or weeping. That has stopped entirely. I had had a 16 mm kidney stone removed. My chemical balance was great, but I was passing only half the fluid I should. I had problems forcing myself to drink enough water. Now I can drink 8 glasses of water with no problem. It remains to be seen but perhaps the kidney stone problems will be no more and were caused by my enlarged prostate.
Ok what are we doing now. I was told not to lift over 15 to 16 pounds for the next 6 months. Well, we have moved back to Chile living in a small cabin in the Andes mountains. It is heated by a wood burning stove. Splitting wood to keep us warm and cook food. I think I have lifted 25 to 35 lbs but not carried such any distance. I do physical work most of an 8 hour day. It is work of my choosing, and I rotate from one task to another depending on how my body feels. Split a little wood, dig a little trench, saw a little wood. Repair a little siding, Take apart old wood, make wooden handles for all the tools without handles, set up large workshop and store wood inside the cabin.
A land of not so many toxins. In a month, you might see a contrail. The worries and pressures of politics are gone. The threat of nuclear war in this area is remote. Food security is good. The air is clean. The water is clean. Most importantly, we are privileged to care of a small native forest.
At 72, we are looking forward to our garden in the spring and living a lot longer here. Chile is a long long way from a lot of things.
Thank you YANANOW!
Some urgency when needing to pee. With mindfulness and Kegels this can be controlled.
In February of 2017, my prostate was removed using the DaVinci robot-assisted surgery with Dr. James Porter at Swedish Medical in Seattle, WA. Since the surgery, I have been cancer free as indicated by my PSA level of .012 taken in July of 2018.
Unexpected positive results were:
1. I am now free from having any leaky lower GI problems as indicated in the past by staining in my undies on occasion.
2. I can now drink the amount of water I need to avoid creating kidney stones.
Side effects:
Lucky me, there was no incontinence, thank you! Dr. Porter. I have somewhat of a problem with urgency. I don't have to go to the bathroom that often but when I do, I must go asap. I have held on for almost the whole day, but only when I have mindful control and do Kegel exercises. Within 6 weeks there was no erectile dysfunction. The sexual experience and climaxing is very different. It is different in that in the past I could tell when I was going to climax and try to control it, and I would know the instant I did climax. Now, I don't know if I'm going to climax and I can't necessarily control it. I am always surprised at climaxing and its intensity. It is more or less an emotional breathtaking experience. There is no feeling of ejaculation of fluid of course.
Details: Understanding angiogenesis is one of the keys to controlling and reversing cancer. Recent research seems to show that growth of blood vessels in the tumor area is cancer promoting.
Cancer, cardiovascular disease, diabetes, inflammation and aging is reversed by reducing stress, eating a 95% whole food, plant based diet and avoiding environmental toxins. The fiber in a whole food, plant based diet helps to rid the body of toxins/oils/fats. Intramyocellular lipids must also be reduced not just body fat. By the reduction of intramyocellular lipids, mitochondria is increased. Also insulin resistance is decreased. My wife and I have reduced the consumption of any processed oils, including extra virgin olive oil, which is the only oil we use sparingly. We eat almost no dairy or other animal products. We eat as much as we want of fresh green vegetables, beans, seeds, nuts, fruit / particularly berries, and whole grains, don't use sugar and try to buy organic or grow our own. Prostate cancer study with Dr. Dean Ornish at the University of San Francisco Medical Center with 20 men shows 19 of them reversing prostate cancer with diet alone.
For more information about reversing prostate cancer, see the following links:
https://nutritionfacts.org/topics/prostate-cancer/ TED Talks https://www.ted.com/talks/william_li/up-next?language=en
William Li: Can we eat to starve cancer? | TED Talk - TED.com
Anyone who would like to talk directly to us about our experience. please feel free to contact us. We have completely changed our lifestyle. It is not an easy thing to do; and on the other hand it is! It continues to be fascinating to learn how dynamic the body is in response to nutrition, exercise and the environment.
YANANOW was unequivocally the most helpful site for studying prostate cancer in all its complexity (and we read a lot of research and studies). My wife and I can not thank you ALL enough, the contributors and the admins over the years who have kept YANANOW going.
We wish you the best.
I'm having difficulty talking about my condition, because it's very good. I'm having survivor's guilt I guess. I realize it's terribly important for people to know of my excellent recovery. My wife and I have diligently studied this disease. I will tell you what procedure we chose, summarize my condition and then give recommendations.
Anyone wishing to have more information is free to contact me.
Procedure: Surgical removal of the prostate, February 2017, at Swedish Urology, Seattle, Washington, by Dr. James Porter using the DaVinci surgical machine.
Decision: The driving factor was an enlarged prostate. The biopsy procedure was guided by using an earlier MRI image. The image was too large to fit on the biopsy screen. 14 biopsy pins were used rather than the standard 12. The weight of my prostate was 9 grams. It was 6 grams heavier than normal. The volume was a factor in my inguinal hernia, large kidney stones, and digestive problems.
Important: The reason for my excellent recovery and health now is because we totally changed our lifestyle, diet and moved to the southern hemisphere.
Recovery: The first 3 days were nightmarish levels of pain. Dr. Porter encouraged me to tough it out with as little pain meds as possible to speed healing. After the catheter was removed, there was no trouble controlling urination. Also I had soft erections.
Current: It has been 3 years now, and my erections are pretty normal. We are creating a bio refuge in Chile. We organic farm doing all of the work manually. I am 75 years old. I cut the grasses with a hand scythe, prepare the organic garden with a wheelbarrow, handcart, ax, broad fork, hoe and rake.
I am on a 95% whole food plant-based diet, thin, no longer an extreme diabetic, free of kidney stones, and not using any medication. Also, I survived 2 heart attacks and reversed my arterial plaque.
Recommendation: Whatever procedure you choose to use you need to change your diet/lifestyle before and after the procedure or it may be useless. We have come to the conclusion that a whole food plant-based diet is a keystone factor. According to research by Dr. Dean Ornish and research cited by Dr. Michael Gregor of nutritionfacts.org, some prostate surgery for cancer can be avoided and/or cancer can be cured with diet/lifestyle. Only in very special conditions should radiation procedures be used in my opinion.
Good luck with whatever path you chose. Remember, always seek out the new research coming down that path. In this regard, Yananow was invaluable. A heartfelt thanks to the people who volunteer and contribute to keep this going.
After 7 years I'm still doing great. I've had no adverse effects.
I have written about my other medical experiences. I had more than just cancer. If interested please read on. I will be improving and editing "My Medical Adventures" in the next YANA update.
Your Are Not Alone now (YANA now) Part 01
BACKGROUND
We (Carl & Jody 56 years) are living high in an Andes mountain forest of the southern hemisphere. We are protecting and promoting the growth of a 65-hectare forest in response to global warming. We left because the toxicity of the northern hemisphere is a serious health problem. When we were children there was a population of two billion. When our children were born there were three billion. There were 9 billion when our daughter gave birth to her youngest. The population growth has come with a growth of extreme inequalities causing a massive number of homeless, sick, and starving.
Growing food has become a highly industrialized massive scale centralized deadly process. This requires massive amounts of capital. It also requires massive plantings of one type of plant. This in turn requires massive amounts of thousands of types of pesticides, herbicides, and fungicides. This has caused the death and injury of thousands of Industrial Farm Workers and brain damage to their children.
We lived in an old farm tank house in Turlock California. No large farm animals exist now because the water was highly contaminated with ammonia fertilizers and other agricultural chemicals.
Our son Turlif would have been brain-damaged if we drank water well. We looked into bottled water and found there were bits of fiberglass from the filters and plastic particles. The water was from the Turlock City water well. It also was contaminated by agricultural chemicals thought to be at safe levels. Deep dive into safe levels and found them known to be toxic because you could measure the damage to babies and older people. However, it was not understood on a molecular cellular just how pesticides herbicides, and fungicides were causing damage. However, it was understood that ammonia fertilizers broke down into nitrites and nitrate salts having free electrons (radicals). They melt the impellers on ammonia pumps and water well pumps no matter what material the impellers are made of. There is no safe level for nitrate or nitrite molecules. What has been said to be safe is when the damage cannot easily be seen or measured. Moreover, no filter can filter them out. The only safe way nitrites and nitrates can be filtered out is by distillation of the water.
We have distilled our water most of our lives, especially in the us. Jody took the first environmental class offered by the University of California system.
We were careful about our food, we thought. Nonetheless, I ended up being overweight, having severe diabetes, kidney stones, two heart attacks, and then cancer. The next medical adventure would be serious forms of dementia. Also, we knew that all types of deadly anti-resistant bacteria, deadly viruses, and fungi. We knew that a plague was in the making. We began to be very suspicious about how safe the food was. It was obvious extreme weather events would first happen in the northern hemisphere. We observed the global weather patterns on earth.net becoming unstable and erratic. This would result in chaotic abnormal weather. It was time to self-activate. When toxic and extreme events became normal we moved to the southern hemisphere.
We purchased a small forest in the mountains. It included a watershed supplying the headwaters of the Quepe River. Four years of living in our forest without electric power was fantastic. We Lived a life somewhat like people did 100 years ago. No restaurants within an hour's drive. The heat was from a wood stove. It was a simple, easy life. Of course, we have only the smallest amount of social security or it would not have been possible.
Many people will say how difficult if not impossible to change lifestyle/diet. It becomes impossible not to change if you change your environment. Even at that, it was a struggle.
First, we needed to understand the culture of Chile. We also wanted to understand what processes and resources existed on the land. People are beginning to understand that the extinction of most life on Earth is a possibility. Some understand the need to change. It is time to try to find other people who want to adopt a plant-based sustainable diet and healthy lifestyle.
We are in the process of creating six one-acre subdivisions. The rest of the one hundred and fifty-six acres is retained as a private watershed and a natural park. Environmental regulations for the future security of water and food will need to be enforced. We believe regulated subdivisions, the creation of a protected watershed, and a forest park offer a possibility of the survival of some local species. We hope this to be inclusive of future children.
The decision to do a deep detail dive into lifestyle change experiences. It would be of better help to people. Unfortunately writing in deep detail is beyond me. However, the challenge is a good one. Accordingly, it will take a long time and many edits.
Core / critical path information: you must understand to be able to make your path to health by supplying your body with what it needs to repair itself.
Mitochondrial dysfunction lies at the core of the diseases discussed here, including common age-related mental diseases such as Alzheimer's and Parkinson's not discussed.
Warning
The subject "how do" from a YANA email prompted me to write more than just a chat in email. The following is a very long "how" and what to "do" with extreme diabetes, blocked arteries, and prostate cancer diseases.
Simply "DO": Eat whole plant-based foods only, Daily exercise, Change your lifestyle to avoid high stress, Avoid all highly processed foods and all environmental toxins.
"HOW TO DO" is not simple, it is very complex. Depending on the health of your biome and microbiome it may require years of effort. Note globally: the air, water, and food supply have been discovered to be toxic. You must understand this is true. Search for all environmental toxins become aware of them and find ways to avoid as many as possible.
"IT IS NEVER TO LATE TO DO" Every cell in your body is replaced within 7 years. Most within a few months. Red blood cells have a lifespan of only 120 days. If you supply the nutrients your body needs to repair itself it can. Your genes can be expressed in many ways and you can change them (epigenetic) in a few days, months or years. You may be able to pass on the changes you have made to your children. The body is so incredibly dynamic it is impossible to fully understand. All medical care will and must become personalized.
A diverse variety of food is necessary. If you have a habit of eating a limited selection of only healthy food is not a good idea. Want to gain weight, you may need to eat some food in a day in an amount, at a time that would not be healthy if done every day.
You need to try to find new combinations every week. You do need to create a 12-hour period where you do not eat any food. It is easy if you do not eat before bed and sleep in. The time you eat different foods, the order in which you eat, how much you eat, their shape, and how they are prepared are as important as what you eat.
Introduction:
We all live in unique biomes. We all have unique microbiomes on and inside our body's digestive tract. Our body is made up of cells. The cells have a nucleus containing DNA. The DNA is a unique combination of our parents' DNA. Living inside the cells of our body are mitochondria cells with different DNA inherited from our mother only. The mitochondrial DNA may not be compatible with the DNA of our cells. The mitochondrial cells create all of the energy for the cells in our body. They are the center of metabolism. It is the location where inputs of sugar, lipids, and insulin are transformed. If the inputs are too high the excess turns to highly Reactive Oxidative Species (ROS) molecules. ROS will rip off electrons from any other molecule/cellular material it comes in contact with. The result is damage and loss of mitochondria increasing insulin resistance, the cause of diabetes. Damage to the cardiovascular system and causing damage to cellular DNA is the cause of Cancer.

The Transformer by Nick Lane is a necessary read to understand the Deep-Chemistry-Life-Death.
You need to know about the Krebs cycle, basic to your metabolism and the origins of life to be able to help your body to repair Itself.
You can avoid, stop, and reverse all of the diseases mentioned above including prostate cancer. If your prostate cancer is too advanced you may need to take Medical emergency procedures. After the emergency medical procedures, you must change your diet and lifestyle so your body can repair itself.
Depending on the emergency medical procedure used, your body will be damaged. It will need to repair itself.
You will need some hardware for biofeedback if you are going to be able to av cancer with a. If and only if you get at a bare minimum hardware and learn how to use it. Scales, thermometers, Blood pressure cuff, blood sugar meter (use at least 3 times a day), and other biofeedback devices need to be used as often as possible. The results are recorded daily with some notation of what you did that day. A minimal health journal. It is a commitment to take care of your body. Start using the devices and learn about how your body responds to the environment (your lifestyle).
You will need to create a medical support team. You need to ask for help. Create a circle of people who are interested in being healthy. The more people who are willing to show up to doctor's appointments or procedures the better you will be treated by the medical professionals.
Carl's e-mail address is: carl AT applied3d.org (replace "AT" with "@")



